I was a kid who dreaded doctor appointments, who would go into the exam room literally shaking, the last kid anyone would have expected to grow up and become a bone marrow or stem cell donor. Whenever I needed blood work or an injection, they would have to enlist extra nurses to hold down my arms, because I couldn’t be trusted not to fight back. My mom used to joke with the doctor that I really made her earn her salary. Worse, Mom used to tease me that if she ever got remarried, she was going to marry a phlebotomist.
Fast forward to 2009. I had just started college, and there was a blood drive on campus. It seemed like all my friends were participating, but I was still terrified of needles and couldn’t see myself volunteering to get stuck with one. Flyers for the blood drive were all over campus, though, and I started to feel guilty. I knew that there was a worldwide shortage of blood and that, because I was young and healthy, I was an ideal donor. I decided it was time to get over this “baby stuff.” As it turned out, that was easier said than done.
It took me about a year before I was able to successfully donate blood. Every time I walked into a blood drive, I would look across the room at the donors lying on the beds and start to hyperventilate, but I just kept going to blood drives and trying to control my anxiety. Eventually, I knew what to expect coming in: what the room would look like, what the information packet would describe, what questions the nurses would ask me, and it started to feel like a familiar environment. I was deferred as a donor a few times for anxiety, a few times for iron deficiency, and once because the nurse couldn’t find my vein. My mom told me I should just give up, that I had tried my best and it was okay not to do this. A Red Cross nurse told me the same thing. But I knew that trying my best wasn’t actually helping anyone, and I was determined to get there – and I did. The day I donated blood for the first time, I was prouder of myself than I’d ever been. What I didn’t know was that this victory was just the beginning.
In 2011, I heard about a bone marrow drive on campus and thought, Why not? It was much less intense than a blood drive. All I had to do was fill out a registration form with my contact information and get my cheek swabbed with a Q-tip. I got my swab, handed in my form, and promptly forgot about the whole thing. In the meantime, life went on: I graduated college, got married, and moved a few times. And then I got a phone call a few days after New Year’s 2015. I had joined the less than one percent of registered donors who are matched to a specific cancer patient.
For me, it was never a question of if I would do it but how I would do it. I knew as soon as I got that phone call that this was not an opportunity I could say no to, even though I understood that it was going to be a complex medical procedure and strictly voluntary. All I knew about my matched patient was that he was a 62-year-old male with MDS (myelodysplastic syndrome), a disorder in which the body fails to produce sufficient blood cells. And I was literally the only person able to give him this gift that could potentially save his life, and there was no way I was going to let that chance get away from me.
The procedure would take place at the Strong Memorial Hospital in Rochester, New York, where we live. There were a lot of preliminary steps I had to take before the procedure itself. First, I had an initial round of blood work to confirm the match and to check for any infectious diseases in my body that would disqualify me from donating. More blood work confirmed that I wasn’t pregnant, another factor that can disqualify a donor. An exhaustive physical exam confirmed that I was generally healthy. Then I had to go back to the hospital to redo the urine sample, which had come up abnormal (the second one was fine), and another round of blood work closer to the date of donation, in case I had become pregnant or contracted an infectious disease since the last test. The sponsoring organization, DKMS, takes this stuff really seriously because so much is at stake. I even got a call from my coordinator shortly before my donation to ask me if there was any possibility that I might be pregnant.
The real work began four days before my donation, when I had to begin daily injections of a drug that would cause my body to produce extra stem cells. The injections were subcutaneous (under the skin) and more painful than a flu shot, and I needed two per day. My first dose was given in the hospital so that I could be monitored in case of an allergic reaction to the drug. I didn’t have a reaction, but I did experience some side effects that prevented me from working for most of that week (nausea on the first day, followed by back pain the rest of the week.) DKMS arranged for a visiting nurse to administer the injections to me at home after the first day.
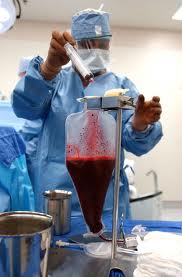
On donation day, my husband and I arrived at the hospital early in the morning. We started with blood work to check my cell count and a final round of injections. Then we went to the apheresis unit, where I was hooked up to a machine that would filter my blood, reserving the stem cells. I had a needle in each arm, one where the blood went out and the other where it was returned, which meant that my range of movement was severely limited. By the time my husband had to leave for work, I had been on the machine for an hour, my tichel was falling off, my shirt was riding up, and I was sweating. I kept shifting my weight, trying to find a comfortable position in the bed, and triggering a series of beeps from the machine letting me know that I was in danger of pulling out one or both of my lines.
There were two male nurses on duty that day. I asked one of them to adjust my tichel. He said he would try, but he didn’t know how I liked to wear it.
“That’s okay,” I told him. “Just as long as my hair is covered. I’m not entering any beauty contests today.”
A local rebbetzin came to visit me in the morning, which was a welcome distraction. After she left, I watched the Food Network for a while, but I was already starting to feel a tingling in my hands and feet associated with low calcium levels in my body, a side effect of the anti-coagulant agent used in the filtering machine. The nurses fed me chocolate calcium chews and pumped extra calcium into my body through the machine, but it wasn’t enough. The tingling progressed to cramping, and my hands contracted into a claw-like shape. I asked for stress balls to curl my fingers around, which helped, but I was still uncomfortable. Eventually, the nurses decided to disconnect me from the machine, even though we had only cycled through 20 liters of my blood (the goal was 24). At this point, I had been hooked up for seven hours and badly needed to use the bathroom.
The nurses warned me that I might be asked to come back and repeat the process the next day in case they hadn’t collected enough stem cells. Apparently, however, the injections had done their job. The lab came back with the results that they had actually collected twice as many cells as they needed!
Once I was discharged, a friend took me out for ice cream and then home. And just like that, it was over. I was more tired than I had been in a long time, and stayed in bed for two days straight. On the third day, I woke up feeling completely normal.
The donation process was a lot more intense than I could have guessed back in 2011 when I so casually put my name down for the registry, but I had a lot of support along the way from my husband and family, my friends, and my DKMS coordinator. Throughout the process, whenever I was feeling scared or in pain, I thought about this: The fact that I was a match for this patient meant that we were probably genetically related in some way, which in turn meant that there was a good chance he was Jewish. So of course I could get through it. I was doing it for mishpacha.
Gila Golder is married to Rob Golder. She grew up in Baltimore and is the daughter of Hannah Heller and the late Craig Heller and the sister of Elliot Heller.






